Toenail Fungus
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment that fungal infections thrive in. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
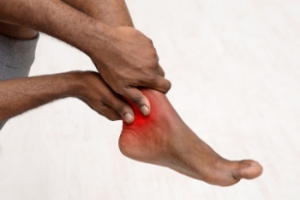
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids and creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
Osteoarthritis of the Ankle
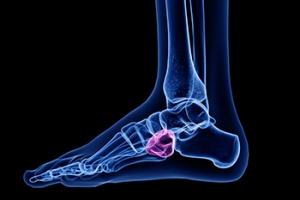
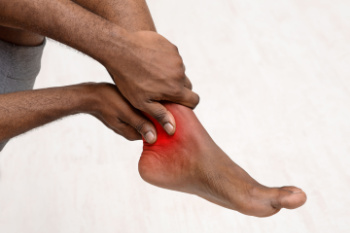 Ankle osteoarthritis is a relatively uncommon condition often arising years after an ankle injury that damages the cartilage. Unlike other forms of arthritis, it tends to affect younger individuals, especially those with a history of trauma to the joint. Excess weight can worsen the condition by increasing stress on the ankle and accelerating cartilage deterioration. Symptoms of ankle osteoarthritis include pain, stiffness, and swelling in the joint, which can increase with activity and improve with rest. Patients may also experience a reduced range of motion and a feeling of instability in the ankle. Diagnosis typically involves a physical examination, patient history, and imaging tests, such as X-rays or MRI scans, to assess cartilage damage and joint space narrowing. Treatment focuses on managing symptoms and improving joint function. Conservative approaches include weight management, targeted stretching exercises, anti-inflammatory medications, and orthotics. In severe cases, surgical options like ankle arthroscopy, fusion, or joint replacement may be considered to alleviate pain and restore mobility. If you have persistent ankle pain, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Ankle osteoarthritis is a relatively uncommon condition often arising years after an ankle injury that damages the cartilage. Unlike other forms of arthritis, it tends to affect younger individuals, especially those with a history of trauma to the joint. Excess weight can worsen the condition by increasing stress on the ankle and accelerating cartilage deterioration. Symptoms of ankle osteoarthritis include pain, stiffness, and swelling in the joint, which can increase with activity and improve with rest. Patients may also experience a reduced range of motion and a feeling of instability in the ankle. Diagnosis typically involves a physical examination, patient history, and imaging tests, such as X-rays or MRI scans, to assess cartilage damage and joint space narrowing. Treatment focuses on managing symptoms and improving joint function. Conservative approaches include weight management, targeted stretching exercises, anti-inflammatory medications, and orthotics. In severe cases, surgical options like ankle arthroscopy, fusion, or joint replacement may be considered to alleviate pain and restore mobility. If you have persistent ankle pain, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions, please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Care for Your Arthritic Foot
Arthritis is an inflammation of the joints and it can occur at any joint in the body, especially in the foot. It generally effects those who are older, however, it can occur at any age. Although there are many different forms of arthritis, there are three main types that occur in the foot. The three types are osteoarthritis, rheumatoid arthritis, and gout.
The primary cause of osteoarthritis is aging. As you age, cartilage degenerates around the joints which causes friction and pain. Obesity can cause osteoarthritis through mechanical stress. Injuries that damage joints can increase the probability as well. Finally, a family history of osteoarthritis can also increase chances of having it.
Rheumatoid arthritis occurs when the immune system attacks the joint linings and weakens them over a long time. While there is no known cause of rheumatoid arthritis, obesity and smoking can increase your chances of getting it. Women are also more likely to get it than men.
Gout is a form of arthritis that occurs when there is too much uric acid in your blood and painful crystals form in your joints. Men are more likely to have gout than women. People who are obese or drink alcohol often are also more likely to develop gout. Furthermore, having diabetes, heart disease, high blood pressure, high cholesterol, gastric bypass surgery or a family history of gout may increase your likelihood of developing the condition.
Symptoms of arthritis include pain, stiffness, swelling in the joints. These symptoms can make it harder and more painful to walk. Physical activity can increase pain and discomfort. Furthermore, joint pain can worsen throughout the day for osteoarthritis. Gout attacks generally last several days with the first few being the worst.
Diagnosis of gout includes either a joint fluid test or a blood test. X-ray imaging can detect osteoarthritis but not gout. On the other hand, there is no blood test for osteoarthritis. Rheumatoid arthritis is difficult to diagnosis. Doctors utilize family and personal medical history, a physical examination, and antibody blood tests to determine if you have rheumatoid arthritis.
Treatment varies for the different kinds of arthritis. Anti-inflammatory medication or steroids can help reduce pain from inflammation of the joints. Changing shoe types can help with some symptoms. Wider shoes can help with discomfort from gout and osteoarthritis. High heels should be avoided. Shoes with proper arch support and that take pressure off the ball of the foot can help with rheumatoid arthritis. Drinking lots of water can also help rid uric acid from the blood. Losing weight, improving your diet, and limiting alcohol and smoking can also help prevent or lessen the symptoms of arthritis.
If you are having trouble walking or pain in your feet, see a podiatrist to check if you have arthritis.
All About Cuboid Syndrome
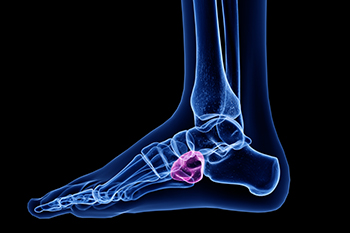 Cuboid syndrome is a condition where the cuboid bone in the foot becomes partially dislocated, causing pain and discomfort. This small bone, located on the outer side of the foot, plays an important role in maintaining the foot's stability and facilitating movement. Causes of cuboid syndrome often include trauma, such as ankle sprains, or repetitive strain from activities like running and jumping. Poorly fitting shoes and biomechanical abnormalities can also contribute to its development. Symptoms typically involve pain on the outer side of the foot, swelling, and difficulty bearing weight. The pain may worsen with physical activity and improve with rest. Diagnosis is primarily based on physical examination and patient history, as X-rays may not always reveal the issue. Treatment involves realigning the cuboid bone through manipulation by a podiatrist, followed by rest, compression, and elevation. Targeted stretching exercises and orthotic inserts may be recommended to prevent recurrence. If you have persistent foot pain, it is suggested that you consult a podiatrist for further evaluation and treatment.
Cuboid syndrome is a condition where the cuboid bone in the foot becomes partially dislocated, causing pain and discomfort. This small bone, located on the outer side of the foot, plays an important role in maintaining the foot's stability and facilitating movement. Causes of cuboid syndrome often include trauma, such as ankle sprains, or repetitive strain from activities like running and jumping. Poorly fitting shoes and biomechanical abnormalities can also contribute to its development. Symptoms typically involve pain on the outer side of the foot, swelling, and difficulty bearing weight. The pain may worsen with physical activity and improve with rest. Diagnosis is primarily based on physical examination and patient history, as X-rays may not always reveal the issue. Treatment involves realigning the cuboid bone through manipulation by a podiatrist, followed by rest, compression, and elevation. Targeted stretching exercises and orthotic inserts may be recommended to prevent recurrence. If you have persistent foot pain, it is suggested that you consult a podiatrist for further evaluation and treatment.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cuboid Syndrome
Cuboid syndrome mostly affects athletes, although it can affect non-athletes too. It is also known as cuboid subluxation or cuboid fault syndrome. This condition occurs when joints and ligaments near the cuboid bone of the foot are damaged, or when the cuboid bone itself is dislodged from its natural position. It is usually marked by pain on the outer side of the foot, which may be persistent or may come and go. Cuboid syndrome can be difficult to diagnose unless it becomes severe and more noticeable. Your doctor will likely ask questions about when the pain began and how long it has been present, and will put pressure on the cuboid bone to determine if that area is the origin of the pain.
Causes of Cuboid Syndrome
- Any repetitive stresses placed on the foot due to athletic activities are a common cause of cuboid syndrome.
- Although it develops over time, it is possible that this syndrome can occur all of sudden due to a single event or injury.
- Over-pronation can exacerbate the condition if not corrected.
Disagreements Amongst Podiatrists Regarding Cuboid Syndrome
- Some refer to it as the dislocation of the calcaneal-cuboid joint only.
- Other podiatrists see it as an injury of the ligaments located nearby, which also involves the cuboid bone.
It is very important that when you experience any kind of pain on the side of your foot, you should seek medical care right away. If a subluxed cuboid is caught early, your feet may respond well to the treatment, and you can get back into sports or other activities again as soon as the pain subsides.
What Can Cause Plantar Fasciitis?
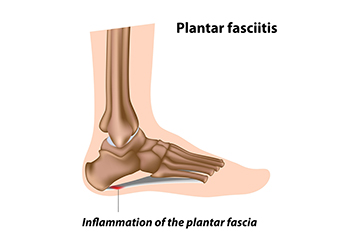
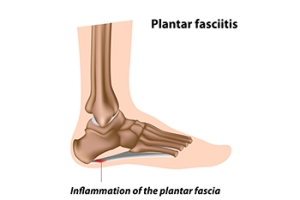
The plantar fascia is a thick band of tissue that connects the heel to the toes. Plantar fasciitis, an inflammation of this tissue, can stem from various biomechanical factors. Problems like an abnormal lower leg structure, limited ankle movement, and inward or outward heel or foot angles can strain the plantar fascia. These abnormalities can alter foot mechanics, leading to excessive tension and micro-tears in the fascia. Symptoms include sharp heel pain, especially after prolonged periods of standing or walking, which tends to improve with rest but worsens upon resuming activity. Early morning stiffness and tenderness in the heel or arch are also common. Addressing these biomechanical issues through proper footwear, orthotics, stretching exercises, and avoiding excessive strain on the feet can help to manage symptoms and prevent recurrence of this ailment. If you have been afflicted by plantar fasciitis, it is suggested that you confer with a podiatrist who can offer you various effective treatment methods.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Symptoms and Treatment of Achilles Tendon Injuries
 Achilles tendon injuries are prevalent among people who engage in physical activities, from athletes to casual exercisers. The Achilles tendon, which connects the calf muscles to the heel bone, is critical for movements like standing on toes and propelling forward when walking or running. Common injuries include Achilles tendinopathy, which involves tiny tears from overuse and results in pain, swelling, and morning stiffness. More severe Achilles tendon injuries, such as partial or complete tears, cause sudden, sharp pain, swelling, and difficulty pointing the foot down or standing on tiptoe. A podiatrist can diagnose these injuries through a physical exam, ultrasound, X-rays, or MRI scans to assess the extent of damage. Treatment depends on the injury's severity. Mild cases may be managed with rest and stretching exercises, while severe tears might require surgery and immobilization with a cast or brace. If you are experiencing pain resulting from an Achilles tendon injury, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Achilles tendon injuries are prevalent among people who engage in physical activities, from athletes to casual exercisers. The Achilles tendon, which connects the calf muscles to the heel bone, is critical for movements like standing on toes and propelling forward when walking or running. Common injuries include Achilles tendinopathy, which involves tiny tears from overuse and results in pain, swelling, and morning stiffness. More severe Achilles tendon injuries, such as partial or complete tears, cause sudden, sharp pain, swelling, and difficulty pointing the foot down or standing on tiptoe. A podiatrist can diagnose these injuries through a physical exam, ultrasound, X-rays, or MRI scans to assess the extent of damage. Treatment depends on the injury's severity. Mild cases may be managed with rest and stretching exercises, while severe tears might require surgery and immobilization with a cast or brace. If you are experiencing pain resulting from an Achilles tendon injury, it is suggested that you schedule an appointment with a podiatrist for an exam, diagnosis, and treatment options.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Pasquale Cancelliere, DPM of Candria Foot and Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
What are Achilles Tendon Injuries
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two injuries. It can be recognized by the following symptoms: inflammation, dull-to-severe pain, increased blood flow to the tendon, thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping. The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising. Problems can also happen among those who do not warm up properly before beginning an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising, you should make sure that the floor you are on is cushioned or has a mat. This will relieve pressure on the heels. A healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region. Further damage could result in severe complications that would make being mobile difficult, if not impossible.