Problematic Flat Feet

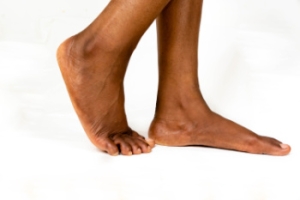
Flat feet, or pes planus, is a condition where the arch of the foot collapses, causing the entire sole to touch the ground. There are two types of flat feet. Flexible flat feet is where the arch appears when the foot is off the ground but flattens when bearing weight. Rigid flat feet is where the arch remains flattened regardless of weight-bearing. Symptoms can include pain, swelling, and fatigue in the feet, ankles, or lower legs. Causes range from genetics and aging to injury, obesity, or conditions like arthritis or diabetes. Flat feet can lead to overpronation, increasing the risk of injuries like plantar fasciitis or shin splints. Diagnosis involves physical examination and sometimes imaging tests like X-rays or CT scans. Treatment options include custom orthotic devices, supportive footwear, stretching exercises, and in severe cases, surgery. With proper management, most individuals with flat feet can lead active lives without significant limitations. If you have flat feet that are causing discomfort, it is suggested that you schedule an appointment with a podiatrist for relief options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flat Feet
Flatfoot is a foot condition in which the arch of the foot has either partially or totally dropped or has never developed. While it is common in babies and small children, it can become a problem for them in adulthood if the arch never forms. For adults, the development of flat feet can be brought upon by injury, as a result of pregnancy due to increased elasticity, or obesity. Those who have health concerns such as rheumatoid arthritis or diabetes may also be at greater risk for developing the condition.
If you suspect that you have flat feet, it is best to consult your podiatrist. Your foot doctor will examine the suspected foot and observe how it looks while you sit and stand. He or she may take an X-ray to determine how serious the condition is. Some common signs of flatfoot include toe drift, in which the toes and front part of the foot point outward, a short Achilles tendon, and a heel that tilts outwardly while the ankle tilts inward.
Once flatfoot has been diagnosed, your podiatrist may suggest one of several treatment options. Flat feet can be rigid, in which the feet appear to have no arch even when the person is not standing; or flexible, in which the person appears to have an arch while not standing, but once standing the arch disappears. Those with flexible flatfoot may be told to reduce any activities that cause pain and to avoid extended periods of walking or standing. Another suggestion may be weight loss, as excessive weight may be placing pressure on the arches
In few cases, if the condition is severe and all other methods have been exhausted surgery may be required. This is normally avoided, however, due to a lengthy recovery time and high cost.
Diagnosis and Treatment of Morton’s Neuroma

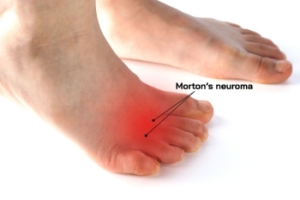
Morton's neuroma is a painful condition characterized by a thickening of the tissue surrounding the nerves leading to the toes, often resulting in a sensation akin to stepping on a pebble. It primarily affects the ball of the foot, typically between the third and fourth toes, and is more common in women and those who wear tight or high-heeled shoes. Prevention strategies include wearing properly fitting footwear with adequate support and cushioning. Diagnosis involves a physical examination, possibly supplemented by imaging tests, such as MRI scans or ultrasounds. Treatment options range from conservative measures such as custom-made orthotics and steroid injections to surgical removal of the affected tissue. If you have this type of foot discomfort, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and treatment plan.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Pasquale Cancelliere, DPM of Candria Foot and Ankle Specialists. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Morton's Neuroma
A neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
Foot Pain From Sciatica

Sciatica is a condition characterized by pain that radiates along the sciatic nerve, which runs from the lower back down through the buttocks and into each leg. When the sciatic nerve becomes compressed or irritated, it can lead to various symptoms, including sharp, shooting pain, tingling, numbness, or weakness in the lower back, buttocks, legs, and feet. In some cases, sciatica can also cause toe pain, often described as a burning sensation or electric shock-like discomfort. This toe pain may result from nerve compression affecting the branches of the sciatic nerve that innervate the feet and toes. A podiatrist can play a vital role in managing sciatica-related foot pain by conducting a comprehensive evaluation to identify contributing factors, providing treatments to alleviate symptoms such as orthotic devices, and coordinating care with other healthcare providers as needed for optimal pain management and functional improvement.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
How Plantar Warts Are Treated
 Plantar warts are caused by the human papillomavirus, or HPV, infecting the skin on the bottom of the feet. These highly contagious warts can be both uncomfortable and persistent. Treatment options vary and may include remedies like salicylic acid, which gradually peels away the wart. A podiatrist, or foot doctor, may suggest more advanced solutions for warts that are more resistant to treatment. Some possible treatments include cryotherapy, which uses liquid nitrogen to freeze and kill the wart tissue, or laser treatment, which destroys the wart with focused light energy. In some cases, minor surgical removal may be necessary, especially for deeper or more stubborn warts. Podiatrists can also provide guidance on preventing the spread of the virus and managing discomfort during the treatment process. If you are struggling with plantar warts, it is suggested that you make an appointment with a podiatrist to discuss treatment options.
Plantar warts are caused by the human papillomavirus, or HPV, infecting the skin on the bottom of the feet. These highly contagious warts can be both uncomfortable and persistent. Treatment options vary and may include remedies like salicylic acid, which gradually peels away the wart. A podiatrist, or foot doctor, may suggest more advanced solutions for warts that are more resistant to treatment. Some possible treatments include cryotherapy, which uses liquid nitrogen to freeze and kill the wart tissue, or laser treatment, which destroys the wart with focused light energy. In some cases, minor surgical removal may be necessary, especially for deeper or more stubborn warts. Podiatrists can also provide guidance on preventing the spread of the virus and managing discomfort during the treatment process. If you are struggling with plantar warts, it is suggested that you make an appointment with a podiatrist to discuss treatment options.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
Caring for Aging Feet

Elderly foot care is imperative due to the profound impact feet have on overall well-being. As the foundation of mobility, feet endure a lifetime of stress and strain, making them vulnerable to age-related changes and conditions. With advancing age, the body undergoes physiological changes, such as decreased skin elasticity and reduced water content in cells, which can contribute to common foot problems like dryness, calluses, and fungal infections. Additionally, structural changes, such as loss of fat padding and decreased circulation, can increase the risk of foot pain, ulcers, and injuries. Regular foot examinations by a podiatrist are essential for seniors to detect and address issues early, preventing complications and maintaining mobility and quality of life. If you are a senior, it is suggested that you schedule routine visits with a podiatrist for guidance and treatment specialized for aging feet.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Pasquale Cancelliere, DPM from Candria Foot and Ankle Specialists. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact our offices located in Londonderry, NH and Salem, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.